OPTIMISING GOAL SETTING FOR PARKINSON'S DISEASE
Researchers at UniSC improve the design of rehabilitation programs for people with Parkinson’s Disease.
Research team: Dr Sarah J. Davies, Dr Hannah L. Gullo, and Dr Emmah Doig
REVIEWERS
Community Science Club
Pomona & District Community House

ARTICLE INFO
Article type: NEW RESEARCH
Issue date: 10/03/2025
Issue No.: 6
Authors: Dr Sarah J Davies, Dr Kathryn M Broadhouse
Original peer reviewed article: https://doi.org/10.1155/2024/9465326
ARTICLE SNAP SHOT
Rationale: why did we do this work? This study investigates the complex and diverse challenges that people with Parkinson’s disease (PD) experience in managing their daily lives with the aim to improve future rehabilitation therapy programs. PD is a brain deteriorating disease that many associate with impaired muscle control, balance and movement.
Novelty: what’s new in this work? However, the findings in this study suggest that non-motor difficulties, to do with the decline of executive cognitive functions (such as memory, low motivation and poor planning skills), are perceived as more restrictive than motor symptoms in daily life.
Relevance: Why does it matter to you? Here, the team examine how people with PD perceive their hurdles and challenges in daily living. By understanding the underlying impairments that impact attainment of goals, the findings of this study offer insights into the needs of people with PD living in the community and can be used to inform the design and content of rehabilitation programs.
INTRODUCTION
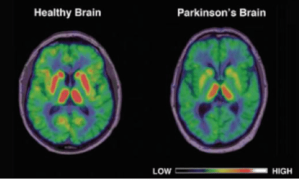
Parkinson’s disease (PD) is a neurodegenerative (brain deteriorating) disease where neurons (brains cells) that control movement, known as motor neurons, become impaired or die. Under normal healthy conditions our motor neurons produce a chemical called dopamine that helps regulate movement and motor learning. However, when these motor neurons become impaired or die they produce less dopamine which then leads to problems with movement. It is this problem with movement that most of us will associate with PD. PD has hallmark effects on muscle control, movement and balance. In fact, people living with PD often have a very specific gait. They take small quick steps and have a tendency to lean forward and keep their arms close to their bodies as well as having trouble initiating and continuing the flow of movement.
While these outward signs of the disease are well known, PD can also cause a wide range of other issues, impairing cognitive ability, senses and mental health. It is this change in cognitive function that includes problems with memory, attention, planning and motivation that can be the most detrimental to peoples’ health and have the most impact on their independence and daily living.
Motor learning
Motor learning is a relatively permanent change in the ability to execute a motor skill as a result of practice or experience
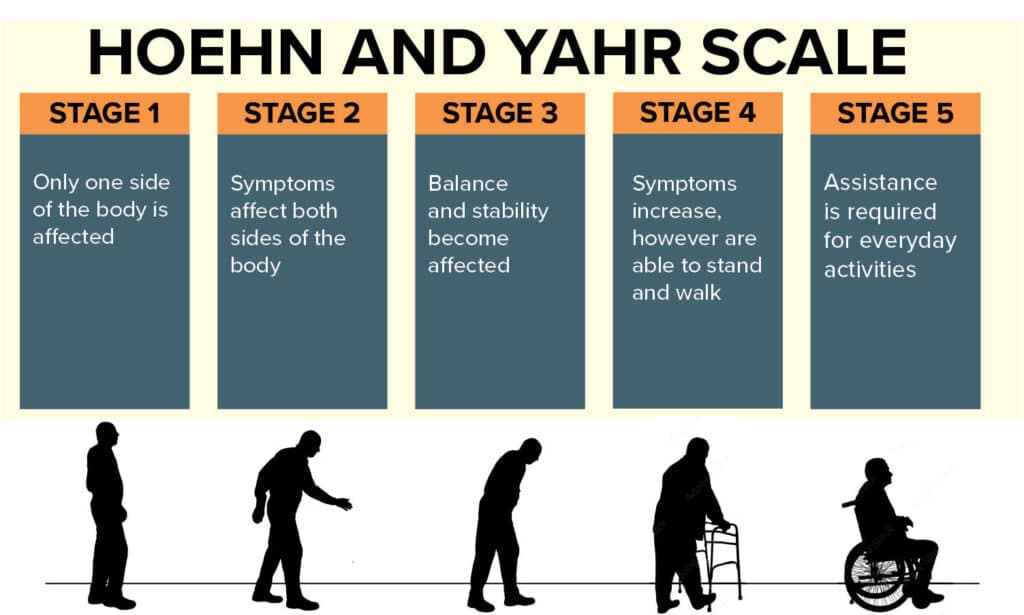
As the disease progresses some people may also develop a type of dementia known as Parkinson’s dementia. There are 5 stages of Parkinson’s. Stages 1 and 2 are considered early PD, stage 3 is the middle stage and 4 to 5 are the advanced stages. Disease progression varies but most people advance through each stage every 2 years except for stage 2 which on average lasts 5 years.
As well as disruption to dopamine production, people with PD also experience impaired norepinephine production. Norepinephrine is the main chemical messenger of the sympathetic nervous system. This system controls your flight or fight response. As such norepinephrine can regulate heart rate, blood pressure, respiratory function and sweat glands. The impairment of norepinephrine with PD is thought to explain some of the non-movement features of the disease such as irregular blood pressure, fatigue and changes in bowl movements.
Researchers still don’t know what causes these brains cells to atrophy and there is currently no cure for PD. Therefore, researchers have turned their attention to 1. understanding risk factors for the disease and 2. improving care and rehabilitation. As an occupational therapist, Sarah and the team’s research focus is in this rehabilitation field.
Sympathetic nervous system
Your sympathetic nervous system is a network of nerves that helps your body activate its “fight-or-flight” response. This system's activity increases when you're stressed, in danger or physically active.
The sympathetic nervous system can accelerate heart rate, widen bronchial passages, decrease motility (movement) of the large intestine, constrict blood vessels, cause pupil dilation, activate goose bumps, start sweating and raise blood pressure.
GOAL SETTING
Goal setting is a core rehabilitation practice for Parkinson’s disease. Targeting therapy towards specific goals set by the individual leads to greater improvements in performance and psychosocial outcomes. Goals direct efforts toward activities that are relevant and meaningful to the person, motivating participation during rehabilitation, driving persistence, and use of task-relevant knowledge and strategies. Both goals and a person’s engagement in goal-setting are important parts of rehabilitation interventions. Research has shown that targeting therapy toward specific goals and engaging patients leads to greater changes in performance for People with Parkinson’s Disease (PwPD) than standardised, impairment-focused approaches.
Goal setting in PD is feasible, and although the nature of goals has been described in previous studies, the underlying impairments that leads individuals to set these goals have not. Understanding the nature of goals PwPD set themselves in rehabilitation ensures that interventions for people with PD are aligned with their needs and priorities. In this study Sarah and the team aim to identify and understand these underlying impairments to highlight which symptoms of PD have the biggest impact on daily life. Elucidating the specific symptoms that underpin person-centered goals will allow individuals and occupational therapists to work together to plan appropriate interventions to target these symptoms and improve daily living.
AIMS
(1) Describe the goals of PwPD
(2) Identify the primary underlying impairment related to each goal selected
(3) Explore whether high- and low-priority goals differed, according to goal type and related underlying impairment.
METHODS
Participants PwPD were recruited to the study if they were able to communicate in English, able to provide informed consent, living in the community and willing to receive the intervention in their homes. People were not eligible to participate if they were diagnosed with a premorbid or current major psychiatric or other neurological disorder, had a diagnosis of dementia or severe cognitive impairment, had a significant sensory impairment (visual or hearing) or a communication disorder which prevented involvement in the intervention and/or reliable completion of outcome measures, were completely dependent on others for personal care and if they were receiving concurrent allied health or cognitive intervention working on the same goals.
Goal setting: Cognitive Orientation (CO-OP)
All participants underwent a goal-setting session to identify their goals, which were targeted using the cognitive orientation to daily occupational performance (CO-OP) intervention. The CO-OP intervention is a frame work occupational therapists use for rehabilitation. It is a task-oriented intervention that uses problem-solving and cognitive strategies to achieve success in patient directed goals. This individualised CO-OP intervention was delivered face-to-face by Sarah who is a CO-OP-certified practitioner in the participants’ homes. The CO-OP contains a series of assessments involving goal setting sessions carried out by each participant and the kind of information/data obtained from each one.
PD REHABILITATION PROGRAMS
Very broadly the 4 main goals of any rehabilitation program are: 1. prevention of the loss of function, 2. slowing the rate of loss of function, 3. Improvement of function and 4. Compensation of loss of function.
The series of assessments are described more fully in an attachment followed by an analysis that addresses each of the three aims listed above and relays the results of the study.
DATA COLLECTION
Identifying goals: COPM
Firstly, Sarah worked with participants to identify and prioritise occupational performance goals in domains of self-care, productivity, and leisure using the COPM assessment. The COPM enables participants to rate the importance of their goals, perceived performance, and satisfaction with performance in goal areas, enabling goals to be prioritized and changes in self-rated performance to be measured. The COPM was used to identify the participant’s goals for their intervention and help rank each of the goals from highest to lowest priority.
Measuring goal attainment: GAS
Next Sarah worked with participants to measure goal attainment using the GAS framework. GASs are scaled using a 5-point measurement scale ranging from − 2 to +2, with baseline performance scaled at − 1 and expected outcomes scaled at zero. − 2 captures the potential for deterioration, and +1 and +2 levels capture the potential for exceeding expected outcomes. The GAS was used in this study to operationalise and scale the goals identified by participants objectively and to document the expected level of achievement by the program end.
Dynamic Performance analysis: DPA
DPA resolves performance issues by identifying performance breakdowns and trialing solutions. It is a dynamic, iterative process carried out by the CO-OP therapist, in this case Sarah, integrating task knowledge, occupational therapy theory, and clinical reasoning to identify effective and ineffective aspects of task performance. Firstly, Sarah assesses whether participants were motivated and knew how to complete the goal-related activities (performer prerequisites). Then the participant was observed or described performing their goal-related activity to identify where and why breakdowns in performance were occurring (performance requisites). The verbal process of guided discovery was then implemented to help participants to “discover” ineffective aspects of task performance and develop strategies to solve them. The participant-derived strategies were then implemented therapeutically, and participants were taught to evaluate their performance to “check” which strategies were effective. Ineffective strategies were discarded, and the process was repeated until an effective strategy was discovered that enabled performance. The effective strategy was then recorded in Sarah’s field notes as the outcome of the DPA.
Demographic data
Demographic information collected from participants included age, sex, disease duration, highest level of formal education, and work status. Evaluations of cognition, perceived cognition, activities of daily living (ADL), PD staging, and premorbid intelligence were also carried out to characterize the participant sample.
Evaluations of cognitive status were carried out using the ACE-III assessment, which assesses 5 neuropsychological domains (orientation and attention, memory, verbal Ruency, language, and visuospatial function) with a cutoff of 88− 77, indicating mild cognitive impairment (MCI).
Perceived Deficits Questionnaire (PDQ) was used to measure participants perceived cognitive status. The PDQ is a self-rated 20-item tool assessing perceived cognitive functioning in four domains (attention, retrospective memory, prospective memory, and planning/organisation). Each item is rated on a 5-point scale Likert scale from 0 (never) to 5 (almost always). A summary score ranging from 0–80 is generated with a higher score indicating greater perceived cognitive impairment.
The Nottingham Extended Activities of Daily Living scale (NEADL) was used to measure activities of daily living (ADL) status. The NEADL consists of 22 items in four subscales (mobility, domestic, kitchen, and leisure). A summary score ranging from 0–22 is generated with higher scores indicating greater independence. The items are rated using a 4-point Likert scale, scored from 0 (not at all, with help) to 1 (on my own with difficulty, on my own) in items representing general ADL tasks.
Disease severity was measured using a modified Hoehn and Yahr (H&Y) scale. The H&Y scale is a 7-point Likert scale that focuses on the functional disability associated with PD. It identifies the progression of the disease through various stages from 1 (unilateral involvement only) to 5 (wheelchair bound or bedridden unless aided). Higher scores indicate more advanced PD.
The National Adult Reading Test (NART]) was used to estimate the premorbid intelligence levels of participants. The NART is a 50-word reading test that provides reliable and valid estimates of intelligence quotient (IQ) and has been shown to be relatively insensitive to the effects of various neurological conditions, including PD.

DATA ANALYSIS
To address aim 1, to describe the nature of the goals of PwPD, Hannah and Emmah, who were not involved with setting goals or delivering the intervention, assessed and coded the COPM goals and GAS goal attainments statements ready for analysis.
To address aim 2, to identify the primary underlying impairments related to the goals, Sarah coded the COPM goals and corresponding performance statements, the DPA. Sarah was the treating therapist in the trial who conducted goal-setting with participants and therefore had knowledge of the participant’s underlying impairments. Through her observations during sessions, goal-setting conversations with participants about why they were having occupational performance problems, as well as the documented DPA, Sarah could make a holistic judgement about the primary underlying PD-related impairments impacting performance.
To address aim 3, to compare differences in goal types and goal-related impairments by goal priority number, the team compared the results for goal type and underlying impairments between goals prioritised from 1 - 4.

RESULTS
Participant Characteristics. Twenty-two participants were included in this study, their characteristics are outlined in Table 1. Participants were on average approximately 5 years postdiagnosis, most had tertiary level qualifications, and most were retired or not working due to their PD condition. The measure of functional independence (NEADL) broadly indicated that the sample had high levels of independence in everyday self-care and domestic activities. Most participants were stage 3 on the H&Y scale, indicating they had mild to moderate bilateral disease with some postural instability but were physically independent. When comparing the study sample with normative data for the ACE-III (cognitive status), 50% were below the norm for healthy controls. Two participants in the study met the criteria for MCI (scores 77–88) on the ACE-III.
ACE-III = Addenbrooke’s cognitive evaluation III; NEADL = Nottingham extended living activities of daily living scale; PDQ= perceived deficits questionnaire; NART =national adult reading test.
Nature of Goals. A total of 88 goals were extracted from the data set and included in the final analysis. The largest proportion of goals were categorised as “self-care” goals. The largest proportion of goals recorded were “managing diet and fitness” goals (n = 17) under “self-care.” the next highest proportion were goals related to “doing housework” (n = 8) under “domestic life,” “recreation and leisure” (n = 8) under “community, social, and civic life,” followed by “completing daily routines” (n = 7) under “general tasks and demands.”
Underlying Impairments Related to Goal Activities. The majority of goals (72.7%) had a primary underlying impairment related to “mental functions” and most of these were categorised as “planning and organisation” or “time management” goals. “Neuromusculoskeletal and movement-related functions” were the primary underlying impairment in 26% of goals and most of these goals were classified as “coordination of voluntary movements” and “control of complex voluntary movements” goals. There was a single “sensory functions and pain” goal in the sample.
Goal Type and Underlying Goal-Related Impairment According to Goal Ranking. For the third aim, Sarah and the team compared proportions of goal types and underlying impairments for PwPD’s highest to lowest priority goals. The goals, regardless of priority, were mostly related to impairments in “mental functions.” Several Activity and Participation categories including “self-care,” “general tasks and demands,” “mobility,” “domestic life,” and “community, social and civic life” were represented across all goals. “Domestic life” goals were the largest proportion of lowest priority goals, whereas “self-care” goals were the largest proportion for higher priority goals.

DISCUSSION
In this study Sarah and the team explored the nature of goals and underlying impairments contributing to goal-related problems of PwPD receiving a community-based rehabilitation program. The nature of goals was diverse, yet primarily related to impairments in “mental functions”, regardless of goal priority. “Self-care” goals made up the greatest proportion of people’s higher priority goals, and “domestic life” goals making up the greatest proportion of their lowest priority goals.
The team found that approximately 73% of the goals in this study were related to impairments in “mental functions,” compared to 26% which were related to “neuromusculoskeletal and movement-related functions”. Research shows that even subtle cognitive impairments influence performance of daily activities which could explain the findings in this study. The smaller proportion “neuromusculoskeletal and movement-related functions” goals could also be because all participants were receiving pharmacological intervention for motor symptom management but that pharmacological treatments are less available or effective for “mental functions” symptoms like executive dysfunction and fatigue. These findings further challenge the view that motor symptoms are the primary problem in PwPD, as the results suggest that nonmotor impairments were more impactful on daily functioning in this group of participants.
Unlike previous studies, participants in this study could select any goals based on challenges they perceived were most important for them to address, which could have been related to cognitive changes, motor changes or other PD-related impairments. Despite this, the goals identified here were consistent with previous literature. Sarah and the team found that PwPD formulated rehabilitation goals to manage their functioning in daily life. The common goal areas across this and previous studies were “self-care,” “general tasks and demands,” “domestic life,” and “community, social, and civic life”.
This reinforces the importance of access to support and community-based rehabilitation services to address activity and participation restrictions.
If we take a look at the “self-care” goals that constituted the largest proportion of all goals in this study, goals under the “managing diet and fitness” accounted for almost 20% of the goals set by participants and 100% of these goals related to commencing and/or maintaining exercise programs. Eighty-five % of the sample set a goal of this nature highlighting the prevalence. Exercise is frequently recommended as a nonpharmacological intervention to protect functioning, manage motor and non-motor symptoms, and to slow disease progression. The predominance of exercise goals in this study indicate that PwPD understand the importance of exercise and aspire to exercise, but that they may need additional supports from their healthcare teams to establish and maintain regular routines to manage their exercise participation around all PD symptoms.
Comparing the nature of goals (aim 1) and related underlying impairments (aim 2) by goal priority (aim 3) provides insights into the motivations, perceived burden of PD symptoms, and priorities of PwPD for rehabilitation. The team found that regardless of priority level, goals were primarily related to impairments in the “mental functions”. This finding is consistent with previous literature and suggests that non-motor difficulties are perceived as more restrictive than motor symptoms in daily life. Participants’ priority goals also represented their motivation to improve or maintain their performance in everyday activities such as exercise, home organisation, time management, and socialisation. These findings offer insights into the perceived needs of PwPD living in the community which may inform the design and content of rehabilitation programs for PwPD.
FUTURE WORK
This study revealed the complex and diverse challenges that PwPD experience in managing their daily lives. By increasing awareness regarding the goals of PwPD, we hope that important clinical and societal outcomes will result, such as novel intervention approaches that meet identified needs and priorities. These findings indicate that non-motor symptoms of executive dysfunction and motivation have a significant impact on performance of, and participation in, a wide array of everyday activities of importance to PwPD, potentially offering guidance to inform the rehabilitation approaches required to meet these needs comprehensively.
Email:HACA@info.edu.au

HACA acknowledges the Traditional Owners of the land on which we conduct our activities. We pay our respect to their Elders past and present and extend that respect to all Aboriginal and Torres Strait Islander peoples throughout Australia
COPYRIGHT © {2023} - HACA