SCARS HEAL BUT NOW WITH THE HELP OF AUSTRALIA’S NATIVE STINGLESS BEES THEY MAY NOT EVEN FORM
The anti-scarring potential of Australia’s native stingless bee cerumen
Research team: Karina D. Hamilton, Daniel Czajkowski, Nicolas J. Kong, Trong D. Tran, Kirk R. Gustafson, Gary Pauly, Glen M. Boyle, Jacinta L. Simmons, Robert Steadman, Ryan Moseley, Peter R. Brooks, Steven M. Ogbourne, and Fraser D. Russell
REVIEWERS
Community Science Club
Pomona & District Community House

ARTICLE INFO
Article type: NEW DISCOVERY
Issue date: 08/07/2024
Issue No.: 3
Authors: Dr Fraser Russell, Dr Kathryn Broadhouse
Original peer reviewed article: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC9404848/
WHY READ THIS ARTICLE?
Scarring is very common after burns, surgery or traumatic injury. Burns patients, military personnel who sustain deep dermal wounds, pedestrians, cyclists, and motorists who are involved in road traffic accidents, sport participants who endure traumatic injuries and women after Caesarean birth may all need anti-scarring therapy during their recovery. Hypertrophic scars, thick, raised scars, can cause itching, contractures, failure to sweat, loss of function, pain and disfigurement and results in major strain on healthcare and workforce productivity. Scarring can also cause significant adverse affects for the individual leading to depression and anxiety.
The global scar treatment market was estimated to be AUD 28 billion in 2022 and is predicted to raise to AUD 47 billion by 2027. The loss of productivity in burn patients with scarring has been estimated at 235 days of absence, costing $33,337 AUD per patient. In contrast to only 46 days of absence in burn patients without scarring, costing almost a fifth of the price, at $6,483 AUD per patient. Existing therapies involve pressure garments, with best outcomes seen when the garments are worn 23 hours a day and in some cases, may need to be worn for up to 2 years! An effective scar therapy, or one that actually stops scars forming in the first place, may save the state millions and save the individual a lot of painful days/months of rehabilitation.
Read on to see how Fraser and the team, with the help of the Australian stingless bee are finding new ways to treat scarring that could have a global impact on scar management.
Contracture
A contracture is a fixed tightening of muscle, tendons, ligaments, or skin. It prevents normal movement of the associated body part. An injury such as a severe burn can cause contracture of the skin.
This should be used as a text description for the video or the Call To Action:
Watch Fraser splitting one of his bee hives
Australian stingless bee, T. carbonaria. The bee is foraging on the Pōhutukawa tree, at the front of Fraser's house in South East Queensland. This species of bee is only 4 mm in length. In the image you can see that the bee is carrying a small amount of pollen in pollen baskets on her hind legs.
Why do we scar in the first place?
Everyone scars. Scarring is evolutionarily advantageous and a consequence of a biological system, in this case the human body, that has learned to respond very quickly to a cut or a wound. Our ancestors whose bodies were better at forming scars were more likely to heal quicker, fight off infection and therefore survive to pass on their genes. Shortly after injury, the body's priority is to seal the wound as quickly as possible. The body’s immune system aims to restore tissue structure and replace lost tissue quickly. Preserving aesthetics and functionality, at this point, is not important; repairing the skin so that it forms an unbroken barrier to the outside world is.
In major injuries, the body's repair mechanisms are unable to restore the skin to its original condition. The result is the formation of inflexible, fibrous scar tissue. This rushed response is great for minimising risk of infection, but unfortunately this can lead to painful scars that dramatically restrict mobility, particularly when muscle and ligament tissue have also been damaged. Scarring is also much more likely to occur in these areas of the body that are under increased mechanical stress, over muscle and ligaments. Compression garments, tight lycra pieces of clothing, can help to reduce scarring by decreasing tension of the skin. However, there is an annoying downside to this therapy; patients need to wear the garment for up to 23 hours per day for 12 to 18 months for it to be effective.
Biological system
A biological system is a group of organs working together to perform a common function. For example, the immune system is a biological system involved with fighting disease and infection, the muscular system is involved with movement, the skeletal system provides protection and support, and the circulatory system delivers nutrients and waste to and from the cells of the body.
INTRODUCTION
The focus of Dr Fraser Russell and team’s work is to investigate and identify novel therapeutic products that inhibit scar formation with the aim of improving recovery and quality of life. To understand the work carried out by Fraser and his team we first need to understand the stages of wound healing and identify key points in this timeline when intervention is possible. We will now take a look at the scarring process itself. Don’t worry, the bees’ involvement will become apparent soon.
To learn more about scar formation flip through the tabs below or watch this short animation
Novel
When we use the word novel in scientific writing we mean that this technique or intervention has not been used or known about before. "New technologies are posing novel problems for our society".
A short animation about scar formation brought to you by HACA
Initial injury
Imagine we have sustained a deep cut on the back of our hand. The wound starts to bleed that will later form a scab. Keratinocytes, the most prolific cell type in skin migrate (move into the wound site), proliferate (multiply), and differentiate (become different in character) to restore our hand’s skin barrier. They do this by growing epithelial tissue, a thin layer of protective cells, over the open wound at the rate of approximately 1mm every 24 hours.
Inflammation stage
Platelets (cell fragments in the blood) in the wound that have caused the blood to clot, bind to collagen in the skin. Collagen is a protein that provides structure, support and strength to our skin, muscles, bones and connective tissue. It is often touted in beauty products as an anti-ageing product as it is responsible for the skin’s elasticity and hydration and not surprisingly, we produce less as we age resulting in, among other things, wrinkles. This “binding” starts a signaling process to alert and recruit cells within the body’s immune system to the wound site to fight local infection. This is the inflammation phase. The wound will appear inflamed, red and perhaps a bit warm to the touch as cells rush into the area.
Proliferation stage
In response to this inflammation, fibroblasts (special collagen-producing cells) at the wound site start laying down more collagen to strengthen the skin. In normal situations fibroblasts deposit collagen in an organized lattice structure that is very strong and elastic. However, when in emergency-response mode, they respond by laying down a lot quickly, in a very unorganized, haphazard way. It is kind of like nailing down a crisscross of two-by-fours over a hole in a roof in a thunderstorm; it seals the hole and stops the rain coming in, but it doesn’t look very nice, is not as structurally sound and does not contain all the components (roof felt, insulation, tiles etc.) as the original roof.
Remodelling stage
The repaired region will contain a lot of collagenous fibers (fibers that provide structure and support to the tissue), and relatively few blood vessels. Damaged sweat and sebaceous glands (glands that secrete an oily substance that protects your skin from drying out), hair follicles, muscle and nerves are rarely repaired. The result is the formation of an inflexible, fibrous white scar that is weaker than normal skin. The problem is that the body doesn’t have a system to go back up on the roof in sunnier weather, rip up the crisscross of collagen two-by-fours and re-lay all the necessary materials for a proper new roof at the wound site (sweat and sebaceous glands, hair follicles, muscles and nerves). We are stuck with it.
"It is this haphazard laying down of collagen, or fibrosis, that Fraser and team are targeting in this paper. If we can intervene and slow the fibroblasts down so they don’t go into panic mode, we can prevent the formation of scars and encourage the slower more meticulous repair of normal tissue."
Scar formation as we age
Our ability to repair damaged tissue to its pre-injury state decreases as we age. We all know this from personal experience; we could all heal a lot faster and efficiently without a noticeable difference in function when we were younger. Remarkably though, it is older skin that may hold the key to scar tissue prevention. As we age the collagen level in our skin decreases. Surgeons have repeatedly noticed that older patients have smaller, thinner scars. This is because fibroblast activity is reduced as we age and responds slower to inflammation. This is not so great from an evolutionary standpoint as we are more susceptible to infection as the wound takes longer to heal and repair, but with modern day medicine and hygiene practices this is not so much of a disadvantage. If we can mimic the older age response to injury and slow down the frenzied laying down of collagen to a more regulated repair, we may be able to manage scar formation, and control rebuilding of all tissue types to minimise final discomfort and maximise mobility when the wound finally heals.
Bring in the bees!
There is a growing interest in the research community to identify novel scar management therapeutics from natural products. Although people have been using honey for millennia for its medicinal benefits, researchers are now looking at bee cerumen (also called propolis by some) for its therapeutic properties. More specifically they are looking at the cerumen from Australia’s native stingless bee, Tetragonula carbonaria. This cerumen is a mixture of wax produced by the bee and resin collected by the bee from trees. Our Aussie stingless bees do not build hives as such, but rather nests (Figure 1). They deposit this cerumen into their nests as it has antibacterial properties and protects the bees from pathogens. Fraser’s team are now looking deeper into the anti-scarring potential of this natural product.
Figure 1 Native stingless bee foraging on nectar (top) and the bee nest (bottom). The brood in the centre of the nest is surrounded by yellow pollen pots and cerumen (propolis). These photos were taken by Fraser of his own hive and at the front of his house.
Pathogen
A bacterium, virus, or other microorganism that can cause disease.
Questions and Answers
REVIEWERS: Is this property/potential of reducing scarring unique to the cerumen of the Australian stingless bees, or is this also true of European stingless bees? If it is just an Australian stingless bee quality, is Australia leading the way in this field?
RESEARCHERS: Australian stingless bee propolis contains Compound 1, which is the compound we have found to have anti-scarring potential in this paper, while European honeybee propolis does not. The anti-scarring potential is unique to our Australian stingless bee propolis. European honeybees and Australian stingless bees exhibit differences in their preference for floral type during foraging. Since the floral source is important to the chemical composition of propolis, the composition of stingless bee propolis is also different to that of the European honeybee. Our research group published a paper in 2011 that described some of the differences in chemical composition (Massaro et al., 2011). Our focus to date has bee on fibrosis of the skin. Yet, fibrosis occurs in other organs, such as the heart following coronary artery disease. Treating fibrosis (scarring) of internal organs such as the heart would be a longer-term objective of this research and would have a global impact.
REVIEWERS: Is there any evidence that people/cultures have already used bee cerumen in scar prevention?
RESEARCHERS: Unfractionated propolis, the "raw" cerumen taken from the hives, contains about 300 hundred different compounds. Studies using unfractionated propolis suggest that this might be efficacious in supporting the immune system and preventing microbial infections. Propolis has been used as an additive in several products, including a moisturiser, toothpaste, soap and food preservative. Our study has fractionated propolis. in the methods below you will see that we have identified and isolated a single compound, Compound 1, that has anti-scarring potential. The application of this compound as an anti-scarring molecule is novel.
METHODS
Now we are all caught up to speed. We will look through this paper that details the work by researchers from UniSC, Brisbane and the UK to investigate the potential of cerumen collected from stingless bee hives in the local Brisbane area to prevent scarring and fibrosis.
Collection and extraction of cerumen
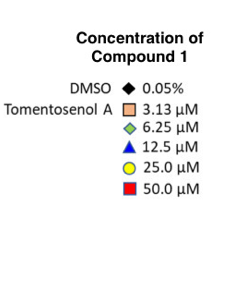
Cerumen was collected from 40 native bee hives in the Brisbane metropolitan region. The research team then isolated the compound Tomentosenol A, in the cerumen, as this is the compound that is thought to have anti-scarring potential. We will refer to Tomentosenol A as Compound 1 from now on. Five different concentrations of Compound 1 were then generated by mixing with a solvent (a liquid that can dissolve other substances). Along with these 5 concentrations a control of just the solvent was created. A control is a bench mark where all variables are kept the same to provide a point of comparison. In this instance the team changed just the concentration of Compound 1 and compared against the Control that contained no Compound 1. We have condensed this information into just one paragraph which doesn’t do justice to the work that went into this. In reality this took hours and hours of painstaking precision, pipetting and trips to the science grade fridge.
Testing on human cells
The team then needed human cells to test the anti-scarring potential of Compound 1. For this they used neonatal foreskin fibroblasts (NFF) and immortal human epidermal keratinocyte cells (HaCaT). Remember from above that fibroblasts lay down collagen and keratinocytes grow a thin layer of protective cells over the open wound. Yes, you did read that correctly, the fibroblasts were taken from neonatal foreskins. Sounds alarming at first glance but neonatal foreskin fibroblasts are readily available due to circumcision and are commonly used in laboratories worldwide. Using cells from foreskin means that no extra procedure to acquire human cells is needed. Immortal human cell lines used for the keratinocyte cell are cells that do not stop dividing, like tumorous cells or cells that have been manipulated to proliferate (multiply) indefinitely. This is a whole other fascinating topic, very briefly, normal cells have a limit to the number of times they can divide and multiple (this is why we can’t live forever). Tumorous cells don’t have this off switch, they just keep multiplying forever. This is terrible for tumour patients but useful in science where we always need cell lines to study.
So we can get to the interesting results, we have glossed over how the team prepare the cell cultures and mix with the concentrations of Compound 1, but it again involves a lot of pipetting, incubation periods in fridges and hours of meticulous work to make sure the two cell cultures of NFFs and HaCaTs are healthy and that everything is the same apart from the concentration of Compound 1.
Tumorous cells
Cells that continually divide forming solid tumours.
Questions and Answers
REVIEWERS: Why did you use neonatal foreskin cells and is circumcision very common?
RESEARCHERS: In the early days of this research, including the study here, we used neonatal human foreskin fibroblasts as a cell type that is relevant to skin. Our decision to use these cells was because they are readily available through a commercial source as circumcision is common in Europe and the USA. We recognise, however, that there are key differences in the neonate and adults in their capacity for scarring. Because of this, our current no longer uses neonatal cells. Our research now uses adult human dermal fibroblasts as a source of normal skin cells, and human hypertrophic scar fibroblasts as a source of hypertrophic scar skin cells. On occasions, we will use some genetically-modified cells to answer specific research questions.
REVIEWERS: can scars disappear?
RESEARCHERS: Some scarring can regress over time, while other scars lead to permanent disfigurement. Contractures resulting from hypertrophic scarring can only be relieved with surgical treatment modalities which reorganize tissue but do not address the underlying cause. Our research aims to identify whether tomentosenol A can prevent scar tissue from forming after deep dermal injury, and whether it can reverse scar tissue once it has formed.
RESULTS
Experiment 1
Cell proliferation
The team first tested cell proliferation when exposed to Compound 1. The team measured the rate at which the NFFs and HaCaTs multiplied every 2 hours over a 72-hour period when exposed to the 5 different concentrations of Compound 1 and in the Control. Remember, in anti-scarring treatment we want to slow down the fibroblasts and keratinocytes so a reduction in the rate of proliferation, the rate at which they multiple, would indicate anti-scarring potential. If we can slow down the number of builders up on the roof, by virtue it will take longer to repair the roof.
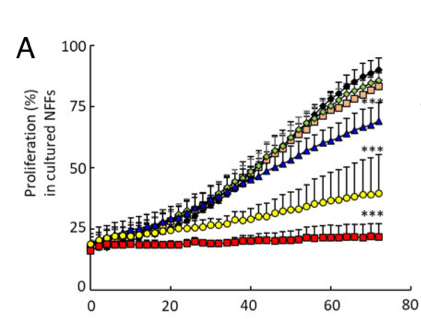
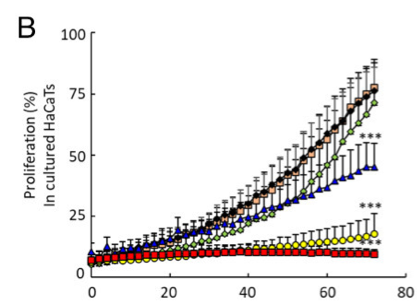
Figure 2A and B show the proliferation rate of NFFs and HaCaTs when exposed to the 5 concentrations and in the Control. On the vertical axis we have proliferation rate (rate at which the cells multiple) and on the horizontal axis we have time in hours. Look at the black diamonds, this is the proliferation rate of the Control, so the benchmark rate at which the NFF and HaCaT cells multiple when not exposed to Compound 1. Now look at the coloured data points, which are the different concentrations. You can clearly see there is increased suppression of cell proliferation with higher concentrations of Compound 1. The red squares represent cell proliferation when exposed to the highest concentration. Both NFF and HaCaT cells have hardly increased in number when exposed to the highest concentrations of Compound 1. This data shows that Compound 1 suppresses cell proliferation and therefore has potential as an anti-scarring treatment.
The *** indicate a statistically significant reduction in cell proliferation with the higher concentrations.
Experiment 2
Wound healing
The team now wanted to understand the effect of Compound 1 on cell migration into a wound site. Remember that when we scratched ourselves in the PCH garden fibroblasts and keratinocytes rushed to the wound site in response to the cut and went into emergency mode. With anti-scarring therapies we are looking to slow down or suppress this cell migration to the wound site. So the team literally created a scratch wound in the cell culture using a Bioscience WoundMaker… (yep, there is such a thing! I googled it and it is not as cool as it sounds, it just looks like a lunch box with a tray inside fitted with micropins that create precision wounds in your cell cultures without damaging the cells or plastic wells they are living in). The team then measured how quickly these wounds healed. They measured the width of the wound again at every 2 hours over a 72-hour period. From this they could derive how quickly the NFFs and HaCaTs migrated into the wound site and closed the wound.
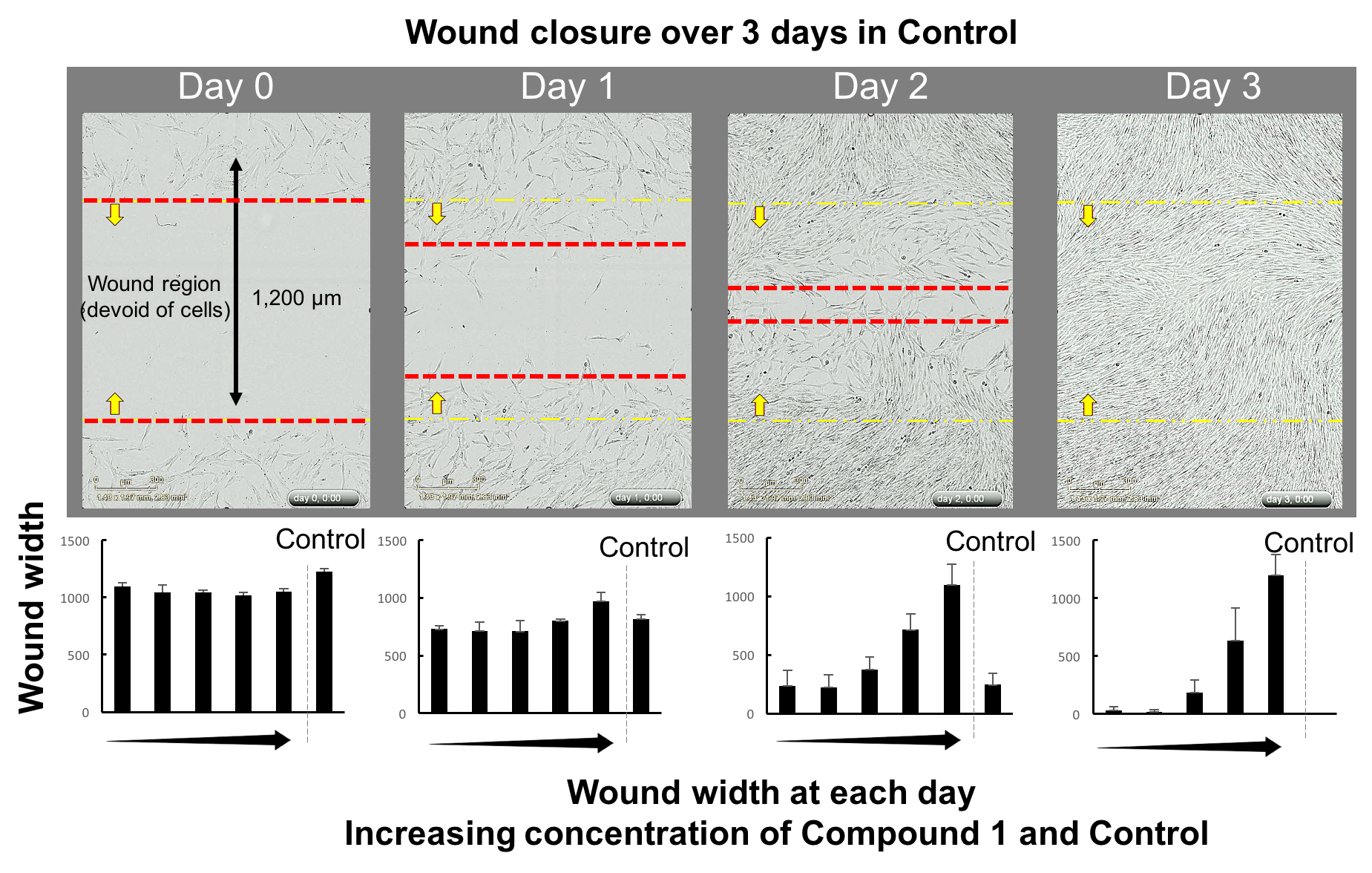
Figure 3: The upper panels show the normal migration of cells without any Compound 1 into a wound region, taken at Day 0 (large wound) through to Day 3 (no wound as cells have migrated to fill the space). The bar graphs underneath each day show the size of the wound with and without Compound 1. At Day 0, the wound is about 1,200 µm distance. After Days 1, 2 and 3, the wound closes with low concentration of Compound 1. However, with the higher concentrations of Compound 1, we can see that there is no reduction in wound size. That is, Compound 1 has prevented the migration of fibroblasts.
By limiting the migration of cells into the wound site Compound 1 may suppress the haphazard emergency-mode fibrotic response.
Experiment 3
Fibroblast activation into emergency mode
As we now know, during the wound healing process fibroblasts are activated into emergency mode and start laying down collagen very quickly. During the wound healing process our bodies send out a signal to activate the fibroblast; a bit like a 000-call alerting the emergency services to an incident. These “activated” fibroblasts can be distinguished from the non-activated fibroblasts as they emit a microfilament known as
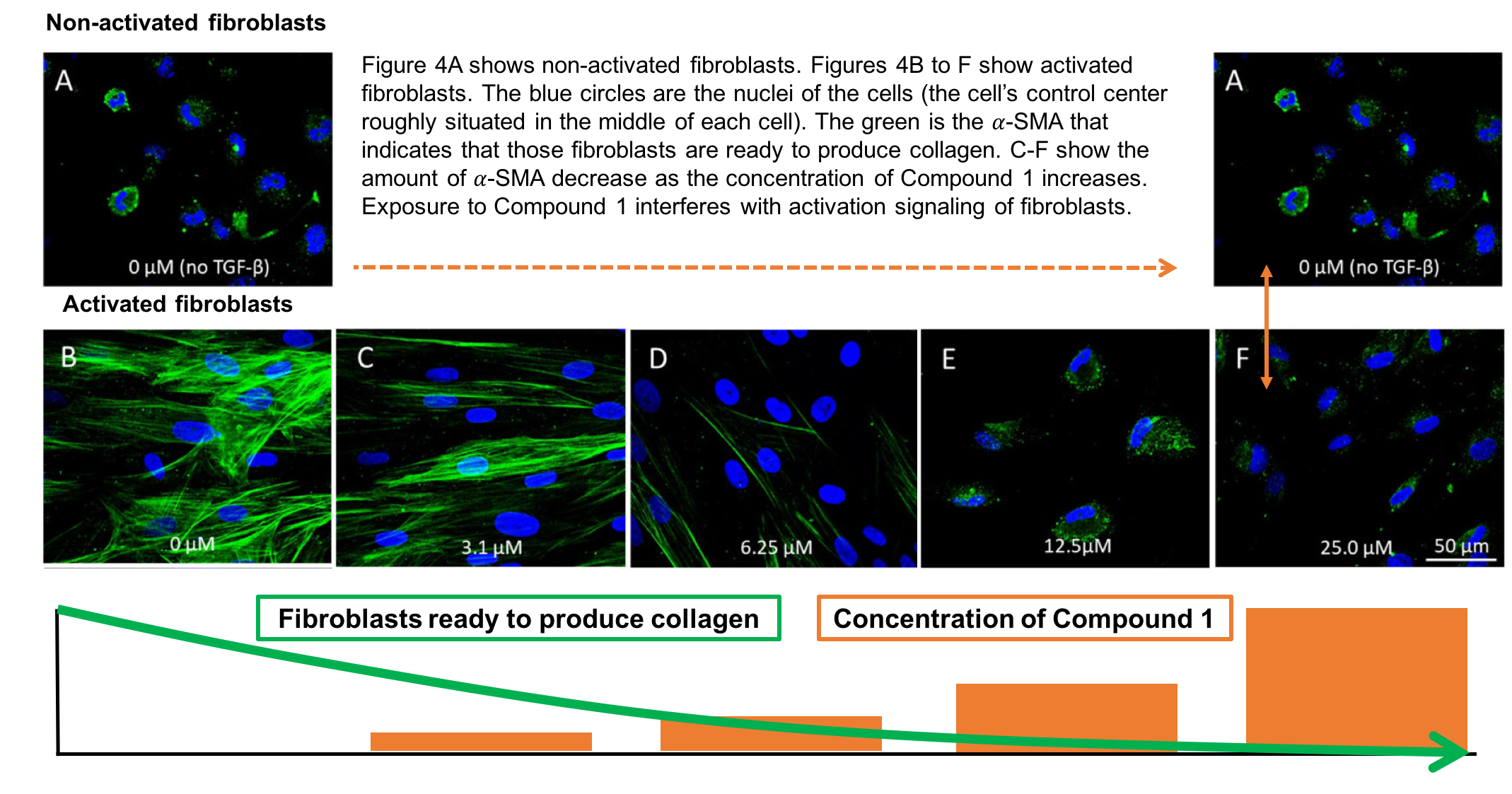
𝛼-SMA when they are ready to start producing collagen. This means we can actually see which fibroblasts are in emergency mode and which are not by looking for the presence of 𝛼-SMA using a confocal microscope. Figure 4 shows 6 images of NFF cells. The samples have been stained to show different parts of the cells. The blue circles are the fibroblasts nuclei; the cell’s control center roughly situated in the middle of each cell.
Figure 4 shows 6 images of NFF cells. The samples have been stained to show different parts of the cells. Figure 4A show NFF cells that have not been activated (the emergency 000 call has not been sent out) and B show fibroblast cells that have been activated to start laying down collagen. You can clearly see the green that marks the presence of 𝛼-SMA indicating fibroblast activation. Now look at C to F. In all images the emergency call has been sent out. However, the team increased the concentration of Compound 1, with C having the lowest and F the highest concentration. You can see that 𝛼-SMA decreases as we increase the concentration of Compound 1. Compound 1 suppresses the activation of fibroblasts and interferes with how they receive and then respond to the 000 call. If the fibroblasts don’t activate then they will not start laying down collagen.
SUMMARY & CONCLUSION
After a lot of hard work from a team of scientists around the world and here on the Coast collecting cerumen, human cell cultures, multiple 3 day stints of painstaking precision measurements every 2 hours and looking down a microscope, the results are in! This study was successful in isolating a small molecule found in nature, Compound 1, that has the potential to prevent scar tissue formation. In the results presented above Tomentosenol A, a compound found in Australian native stingless bee hives has been proven to:-
1. Slow down cell proliferation. Compound 1 reduces the rate at which cells multiply at a wound site.
2. Inhibit cell migration to the wound site and therefore slow down the wound healing process.
3. Interferes with the body’s signalling process that activates fibroblasts to produce collagen, which then reduces the frenzied laying down of collagen.
QUESTIONS & ANSWERS
REVIEWERS: How would this treatment be administered, if proven to be efficacious in human trials? A balm, cream or injection?
RESEARCHERS: Our trial in animals involves administration of microinjections of Compound 1 (tomentosenol A) into the skin. If this research progresses to clinical trials, we will engage with industry experts to formulate the compound as a cream for administration to the surface of the skin. We decided to use microinjections initially, as we want to be sure that the compound penetrates the skin surface.
ONGOING WORK
"We are currently undertaking studies that are aimed at understanding how Compound 1 produces the effects seen in this study. We have made some headway in this space. Lisa Randall is a PhD candidate whose sole focus is reveal the mechanism of action of Compound 1. While knowledge of mechanism is not an absolute requirement for TGA (herapeutic goods administration) approval, it is very helpful to have this information. If we understand how the agent works, we can better predict unwanted effects and potential interactions with other drugs or nutrients. The next step will be a pre-clinical trial in which we administer Compound 1 to an animal model of hypertrophic scarring. Researchers at the University of South Australia developed a mouse model of scarring that is caused by long-term infusion of a particular antibiotic (bleomycin) into the skin. We will use this model to test the efficacy of Compound 1 to prevent and to reverse hypertrophic scars."
Dr Fraser Russell
FUTURE WORK
The results published in the original scientific peer reviewed article online and translated here are a really promising start, but it’s not quite time to rush and collect our own stash of stingless bee cerumen. Fraser and the team have looked at the effect of Compound 1 on two of the most critical cells for wound repair and scar formation, fibroblasts and keratinocytes, in a controlled environment in the lab. A sterile lab is a million miles away from the complex chaotic environment of a human body. In reality, in the body, wound healing and scar tissue formation are highly orchestrated events that require multiple cellular interactions. However, these highly controlled experiments are needed to start to understand the potential of Compound 1. When we don’t know anything about the therapeutic effects of a compound we first need to alter one variable at a time to isolate the effects of that change. It is therefore possible that the efficacy of stingless bee cerumen may be different in a complex environment such as the human body. The next step is to test Compound 1 in animal models and then finally, human subjects. There is a lot more work ahead, but stingless bee cerumen could potentially provide a natural therapeutic treatment for scar prevention, facilitating patients’ recovery to near pre-injury levels of mobility and function.
QUESTIONS & ANSWERS
REVIEWERS: If this treatment was proven to be efficacious in human trials, would compound 1 be synthesised in the lab? How would these research findings move to a pharmaceutical product?
RESEARCHERS: Compound A is very difficult to synthesise. The chemists in our group have managed to do this, but the yield is very small. It is likely that Compound 1 would be extracted from the natural product rather than synthesised in the lab. The typical path to development of a pharmaceutical is - 1. discovery, 2. preclinical research, 3. clinical trials and 4. approval by the government regulator (in Australia, this is the therapeutic goods administration, TGA). The path to pharmaceutic product would entail several key steps.
- We need to formulate Compound 1 so that it can be administered by application of a dermal cream rather than an injectable agent. Once formulated, we would need to carry out experiments to ensure that the compound penetrates the deep dermal layers of the skin (that is, ensure that it reaches its target site).
- We have already undertaken an assessment of compound stability and have found that Compound 1 is stable when stored over a period of 30 days.
- We would need to carry out cytotoxicity screens (a process to evaluate living cells reaction to a substance and whether it is harmful of not) and determine compound safety when administered to humans. Although unfractionated propolis (the raw cerumen from the hive) is marketed by companies such as Comvita as an oral spray, we would need to undertake an assessment of safety for our isolated compound.
- Consistency in product is important and so we would need to be able to minimise batch-to-batch variability in product.
- Prior to testing in animals or humans, we would need to apply to an Animal Ethics Committee, or a Human Research Ethics Committee for approval. Each application can take several months to develop and go through the approval process. If the project evolves to a clinical trial that is run at a hospital, we will also require Hospital Research Governance approval. This is also a lengthy process that can take several months to complete.
- Depending on the outcomes that are being tested, we would need collaboration with a wound-healing clinic to undertake clinical trials. Our research group has established a connection with a major wound healing unit in Sydney. This collaboration is very much in its infancy.
Email:HACAinfo@usc.edu.au

HACA acknowledges the Traditional Owners of the land on which we conduct our activities. We pay our respect to their Elders past and present and extend that respect to all Aboriginal and Torres Strait Islander peoples throughout Australia
COPYRIGHT © {2023} - HACA